Dystrophy (Muscle Disease)
What is Muscle Disease (Dystrophy)?
In the medical language, muscle diseases are called muscles dystrophy. The word dystrophy is derived from ancient Greek by the combination of the words dis, meaning bad, diseased, and trophy, meaning nutrition, development. Muscular dystrophies (muscular dystrophies) have no definitive treatment. However, medications and therapies can help manage symptoms and slow down the course of the disease.
There are more than 30 muscle type dystrophies and each of these dystrophies may vary according to the following characteristics:
- Genes causing the disease,
- Muscles affected,
- The age at which symptoms first appear,
- The rate of progression of the disease.
The most common muscle dystrophies are as follows:
Duchenne muscular dystrophy (DMD): It is the most common form of muscle dystrophies. It mainly affects boys and starts between 3 and 5 years of age.
Becker muscle dystrophy: Similar to Duchenne muscular dystrophy, but symptoms are milder and age at onset is later. Symptoms of the disease affecting boys occur between the ages of 11 to 25 years.
Myotonic muscular dystrophy: It is the most common muscle disease in adults. Individuals with myotonic dystrophy have difficulty loosening their muscles after cushioning (for example, loosening hands after shaking hands). It can affect both men and women.
Congenital muscular dystrophy: It starts from birth or within the first two years. It can be seen in both sexes. Some forms progress heavily, while some forms tend to be lighter.
Limb-Girdle muscular dystrophy with limb involvement: It usually involves the muscles around the shoulder and hip.
Facioscapulohumeral muscle dystrophy: It affects the facial muscles, shoulders and upper arms. It can affect people of all ages, from young people to adults.
Distal muscular dystrophy: Affects muscles of arms, legs, hands and feet.
Oculopharyngeal muscular dystrophy: It causes weakness in the muscles of the face, neck and shoulder, sagging eyelids (ptosis), followed by difficulty in swallowing (difficulty swallowing).
Emery-Dreifuss muscular dystrophy: It usually affects men. It causes heart problems along with muscle weakness.
Inheritance of Muscular Dystrophy
Muscle dystrophy may be hereditary or may occur due to a mutation in one of the genes. This is a rare condition. Mutations causing muscle dystrophy are observed in genes encoding proteins that keep muscles healthy and strong. For example, in those with Duchenne or Becker muscle dystrophies, the protein called dystrophin, which strengthens the muscles and protects against injury, is insufficient.
What are the Symptoms of Muscle Disease?
In most muscle dystrophies, symptoms begin to appear in childhood or adolescence.
- Fall often,
- Having weak muscles,
- Muscle cramps,
- Difficulty getting up, climbing stairs, running or jumping,
- Walking on your toes,
- Having a curved spine (scoliosis),
- Drooping eyelids,
- Heart problems,
- Shortage of breathing or swallowing,
- Vision problems,
- Weakness in the facial muscles.
How is Muscle Disease Diagnosed?
To make a diagnosis of muscular dystrophy, the specialist physician first performs a physical examination. He then receives a detailed medical history from the patient. Several tests may be required for the diagnosis of muscular dystrophies. Some of them can be listed as follows;
Electromyography or EMG: Small needles called electrodes are placed in different parts of the body and the patient is asked to slowly flex or relax their muscles. The electrodes are connected by wires to a machine that measures electrical activity.
Muscle biopsy: A small piece of muscle tissue is removed using a needle. This fragment is examined in the laboratory to determine which proteins are missing or damaged. This test can show the type of muscular dystrophy.
Muscle strength, reflexes, and coordination tests: These tests help doctors eliminate other nervous system-related diseases.
Electrocardiogram or ECG: Measures electrical signals from the heart and determines how fast the heartbeats and whether it has a healthy rhythm.
Other imaging techniques: For the diagnosis of muscle diseases, imaging methods such as MRI and ultrasound, which show the quality and quantity of muscle in the body, may be used.
Blood testing: Doctors may also request a blood sample to look for genes that cause muscular dystrophy.
How is Muscle Disease Treatment Done?
It has options to improve symptoms and improve the patient’s quality of life. Some treatment methods that improve the patient’s quality of life in muscle dystrophies are as follows;
Physical therapy: Different exercises are used to keep muscles strong and flexible.
Speech therapy: Patients with weak tongue and facial muscles can be taught easier ways to talk with speech therapy.
Respiratory therapy: In patients with difficulty in breathing due to muscle weakness, ways of facilitating breathing or the use of respiratory support machines are shown.
Surgical treatments: Surgical treatments can be used to reduce the complications of muscular dystrophy such as heart problems or swallowing difficulties.
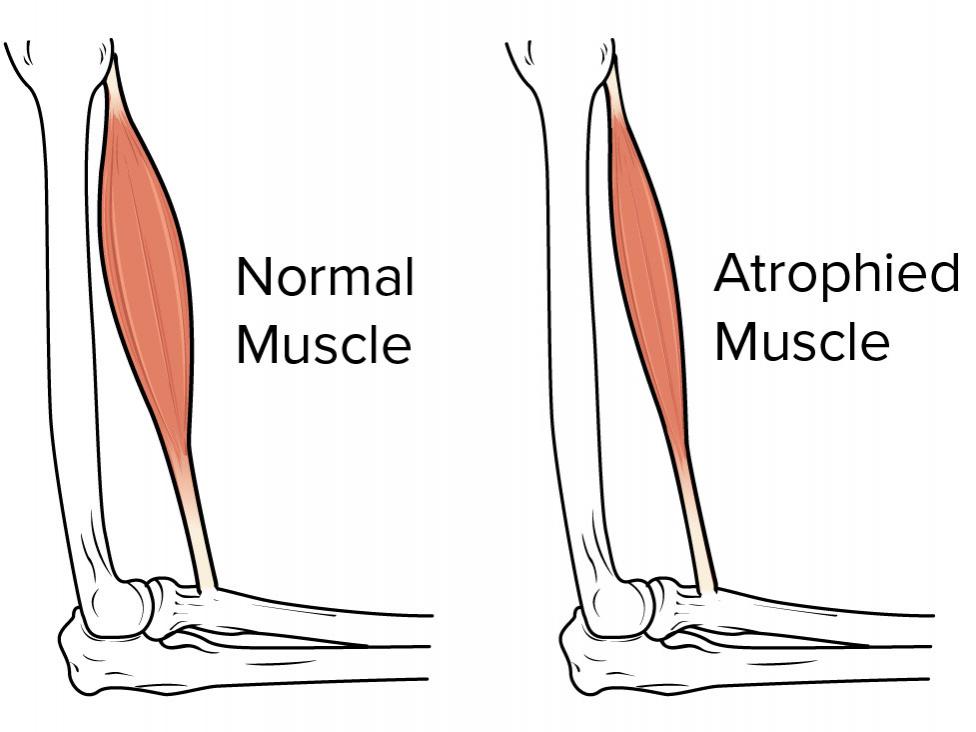
Muscle Atrophy (Muscle Loss)
Muscle atrophy refers to the condition in which the muscles gradually decrease and wear. The main cause of muscle loss is the lack of physical activity. Muscle loss can occur when a disease or disability makes it difficult or impossible to move your arm or leg.
What is Muscle Atrophy Symptoms?
- The following conditions indicate that you may have muscle atrophy:
- Significantly smaller than one of your arms or legs
- A significant weakness of a limb
- Not being physically active for too long
If you think you may have muscle atrophy or cannot move normally, you should have a complete medical examination. Because you may have an undiagnosed condition that requires treatment. Your doctor will provide you with the appropriate diet and exercise options.
What Causes Muscle Atrophy?
If you are not mobile during the day, unused muscles may be lost. Even then, this problem can often be reversed by exercise and nutrition. Atrophy can also occur if you are tied to a bed or cannot move some body parts due to a medical condition.
Other causes of muscle atrophy include:
- Lack of physical activity for a long time,
- Ageing,
- Alcohol-related myopathy, pain and weakness in muscles due to excessive use of alcohol for a long time,
- Burns,
- Injuries such as a torn rotator sheath or bone fracture,
- Not enough feeding,
- Spinal cord or peripheral nerve injuries,
- Stroke (stroke),
- Long-term corticosteroid therapy can be listed as causes.
Some diseases can also cause muscular wear or make movement difficult, causing muscle atrophy. Some of them are listed below:
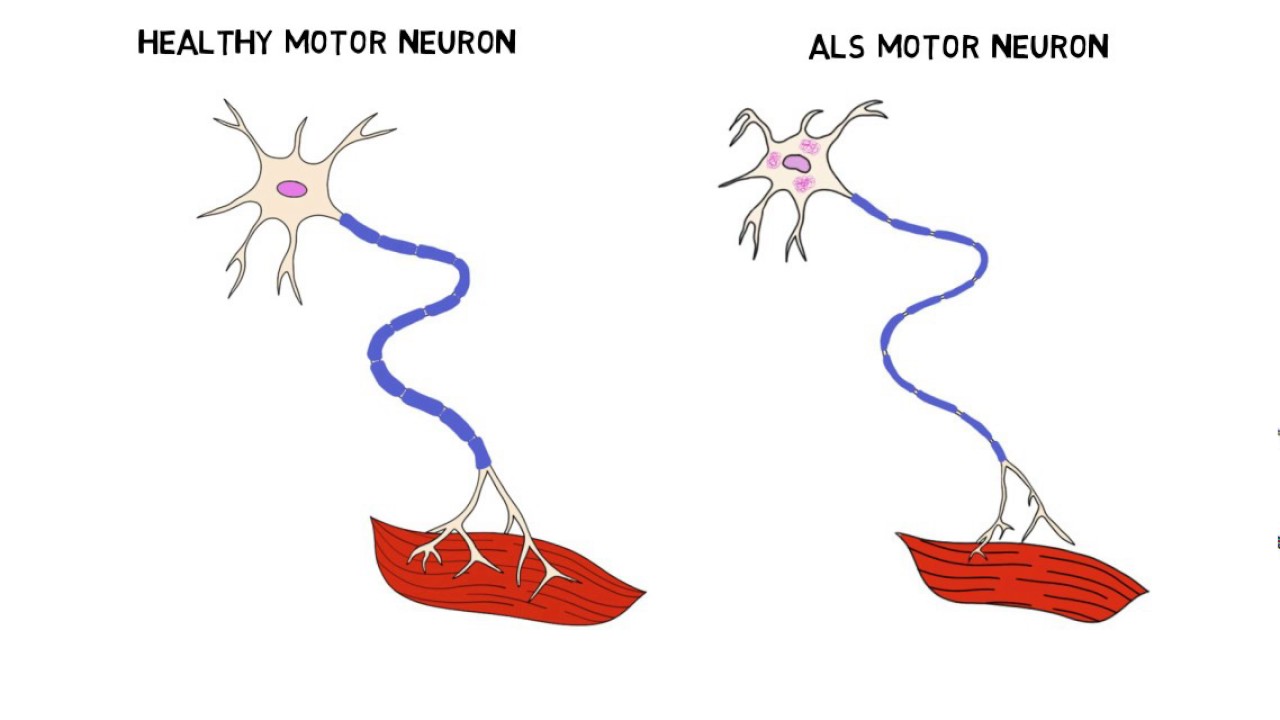
- Amyotrophic lateral sclerosis (ALS), also known as Lou Gehrig’s disease, affects nerve cells that control voluntary muscle movement.
- Dermatomyositis causes muscle weakness and skin rash
- Guillain-Barré syndrome is an autoimmune disease that causes nerve inflammation and muscle weakness.
- Multiple sclerosis is an autoimmune disease in which the body destroys the protective coatings of the nerves.
- Muscular dystrophy is an inherited disease that causes muscle weakness.
- Neuropathy can damage a nerve or a group of nerves, causing sensory or functional loss.
- Osteoarthritis causes reduced motion in the joints.
- Polymyositis is an inflammatory disease.
- Rheumatoid arthritis is a chronic inflammatory disease affecting the joints.
- Spinal muscular atrophy is an inherited disease that causes the wear of the arm and leg muscles.
How is Muscle Atrophy Diagnosed?
Your doctor will ask for your complete medical history. You should tell them about old or recent injuries and previously diagnosed medical conditions. Make a list of the medications you take and give a detailed description of your symptoms.
- Blood tests,
- X-ray film
- Magnetic resonance imaging (MRI),
- Computed tomography (CT) scanning,
- Nerve conduction studies,
- Muscle or nerve biopsy,
- Electromyography (EMG) can be performed.
How is Muscle Atrophy Treated?
The treatment of atrophy, a muscle disease, varies depending on the diagnosis and severity of your muscle loss. In this process, the underlying medical condition needs to be addressed.
Common treatments for muscle atrophy include:
- Exercise,
- Physiotherapy,
- Ultrasound therapy,
- Surgical intervention,
- Nutritional changes can produce good results.
Ultrasound therapy is a noninvasive procedure that uses sound waves to aid healing. Surgical intervention may also be required if your tendons, ligaments, skin or muscles are too tight and prevent you from moving.
If muscle atrophy is caused by malnutrition, the surgical procedure may improve contracture deformity. A torn tendon may cause muscle atrophy, but this problem can also be corrected by surgery. Your doctor will advise you to eat properly and recommend appropriate nutritional supplements if necessary.
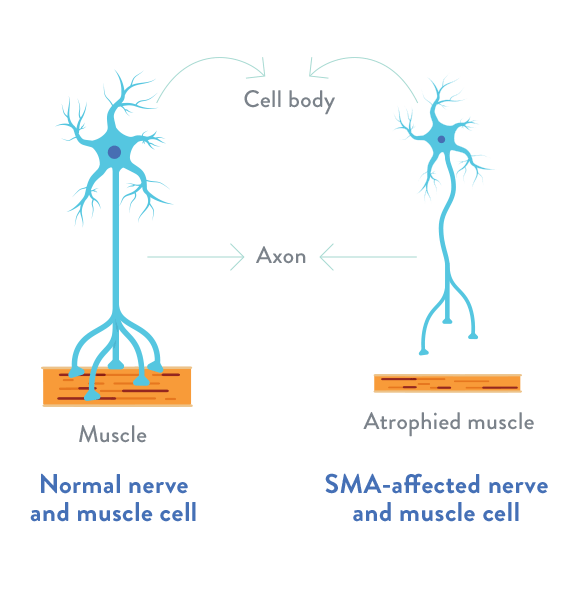
Spinal Muscular Atrophy (SMA)
What is SMA?
Spinal Muscular Atrophy (SMA) is a neuromuscular disease caused by movement nerve cells (motor neurons). The most dangerous of SMA is the stage SMA Type 1.
What are the types of SMA?
The four types of SMA are classified according to the severity of the disease and the age at which symptoms begin:
- Type I is sometimes referred to as infantile-onset SMA or Werdnig-Hoffmann’s disease. Type I begins to affect infants from birth to 6 months, most infants show signs of illness for 3 months. This is the heaviest form of SMA.
- Type II begins to affect children aged 7-18 months. Children can sit independently, but cannot walk. This form can be more severe with moderate.
- Type III is also called Kugelberg-Welander syndrome or pediatric SMA. He begins to influence children at 18 months of age or adolescence. Children can walk independently, but there is a weakness in their arms and legs and may fall frequently. This is the lightest form of SMA in children.
- Type IV is an adult form of SMA. Symptoms usually begin after the age of 35 and gradually worsen over time. Because it develops slowly, many people with type IV SMA do not know that they have SMA until years after the onset of symptoms.
What is SMA Symptoms?
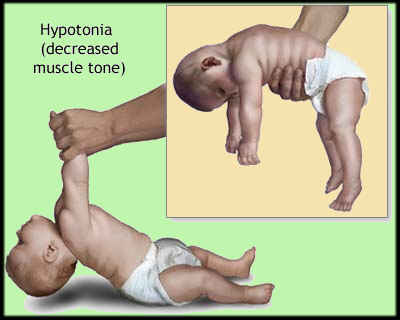
SMA symptoms depend on the severity and age of the person when it starts. Infants with SMA type I are born with very little muscle tone, weak muscles and feeding and breathing problems. With SMA type III, symptoms may not appear until the second year of life.
In all its forms, the main feature of SMA is muscle weakness associated with muscle atrophy.
- Weak muscles and weakness leading to lack of motor development
- Reduced reflexes
- Shaking hands
- Inability to maintain head control
- Nutritional difficulty
- Skinny sound and weak cough
- Cramping and loss of walking ability
- Dating back from peers
- Frequent falls
- Difficulty sitting, standing and walking
- Language twitching
How is SMA Disease Understood?
Since spinal muscular atrophy affects movement and nerve cells, bilateral weakness is usually recognized when there is the limitation of movement. SMA occurs when the mutated gene passes from both parents to the baby when parents decide to have a baby in their life without realizing that they are carriers. In the case of genetic transmission from one of the parents, the carrier may occur even if the disease does not occur.
When the parents consult the physician when they notice abnormalities in the movements of their babies, nerve and muscle measurements are made with EMG. When abnormal findings are detected, suspicious genes are examined by blood test and diagnosed as SMA.
How is SMA Treated?
There is no definitive treatment for SMA yet, but the studies are continuing at full speed. However, different treatments to reduce the symptoms of the disease can be applied by a specialist physician to improve the patient’s quality of life.
Raising the awareness of the relatives of the patients diagnosed with SMA on care, facilitating home care and improving the quality of life of the patient plays an important role. Since Type-1 and Type-2 SMA patients are usually lost due to lung infections, it is very important to clear the airways of the patient if the breathing is irregular and insufficient.
ALS (Amyotrophic Lateral Sclerosis)
What is ALS?
ALS is a progressive neurological disease. ALS is defined as the progressive degeneration of motor nerve cells in the brain and spinal cord. When motor neurons fail to send impulses to muscles, muscle weakness begins. ALS disease often referred to as a syndrome, may show different appearances.
Causes of ALS Disease
The exact cause of ALS is unknown, but several risk factors have been identified:
Genetic: More than 130 genetic alterations have been detected in ALS patients, but the deterioration in the structure of the gene encoding the superoxide dismutase (SOD) enzyme found on chromosome 21 is the most common.
Glutamate excess: The substance ‘glutamate’, which has an important role in nerve transmission in the brain, was found to have higher levels than normal in ALS patients. Excessive glueing of glutamate damages nerve cells.
Impairment of cell metabolism: Every cell has transport systems that bring nutrients and chemical compounds to the cell and also transport waste. Disruption of these waste transport systems in motor nerve diseases disrupts nerve functions.
Oxidative stress: Various types of oxygen formed during cellular metabolism damage intracellular structures, causing cell damage and cell death.
Autoimmune causes: Nerve cell death may occur as a person’s immune system attacks their nerve cells.
Age: The risk of developing the disease increases with age. It is most commonly between the ages of 40-60.
Environmental factors: Smoking, exposure to heavy metals such as lead, mercury, aluminium, infection, exposure to the electromagnetic field, head trauma.
ALS Symptoms
As ALS progresses, the following symptoms become more pronounced;
- Muscle twitching and cramping, especially in the hands and feet
- Disruption in the use of arms and legs,
- Weakness and weakness,
- Weight loss.
When ALS progresses, the following symptoms occur:
- Shortness of breath,
- Difficulty breathing and swallowing.
What are ALS Types?
Classic ALS: Described and progressed by damage to the upper and lower motor neurons. Two-thirds of people with ALS have this type.
Primary lateral sclerosis: It is seen with the disorder of the upper motor nerve cells.
Progressive bulbar palsy (PBP): Lower motor nerve cell disruption; difficulties in speaking, chewing and swallowing begin. ALS affects 25 per cent of patients.
Progressive muscular atrophy (PMA): It is seen by disruption of lower motor neurons. If the upper motor neurons are not affected within two years, they usually remain as lower neuron disease.
How is ALS Diagnosed?
A complete physical examination and medical history of the person is required for the diagnosis of ALS. Some laboratory and radiological tests are also performed to confirm the diagnosis;
- EMG test
- Blood test
- Cerebrospinal fluid examination
- Mar
For ALS Treatment
Certain methods are used in the treatment of ALS. ALS treatment can be listed as follows:
- Medications are given to relieve painful muscle cramps, excessive saliva and other ALS symptoms.
- Maintaining one’s mobility; Physical therapy is applied to relieve muscle stiffness, cramping and fluid retention.
- When swallowing difficulties occur, good nutrition, encouragement and other nutritional options are recommended.
- Speech therapy and communication training to maintain as many verbal communication skills as possible. There are also non-verbal techniques in communication education.
- Aids are used to support daily activities such as dressing, eating, toilets and bathing.
- Used as a wheelchair, air mattress, mattress and equipment to help individual movement.
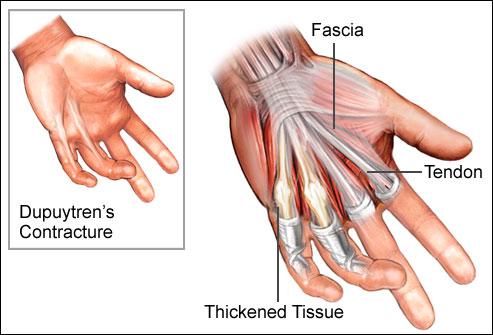
Dupuytren’s Contracture
What is it?
Dupuytren’s disease; It is a disease caused by thickening of the layer called a fascia altında under the skin, often on the palm. Due to the thickening of the fascia as a result of the disease, wrinkling of the skin and tendon adhesion occurs.
What Are The Reasons?
Although the exact cause is not known, it is thought to be the result of biochemical changes in the fascia. Often; occurs in both hands, men over 40 years of age and people of northern European origin. The incidence of the disease increases in diabetics and alcoholics.
Let us briefly list the risk factors that cause Dupuytren’s contracture;
- I alcoholysis
- Diabetes
- Epilepsy (epilepsy)
- Vascular diseases
- Genetic factors
- Senile
What are the Symptoms?
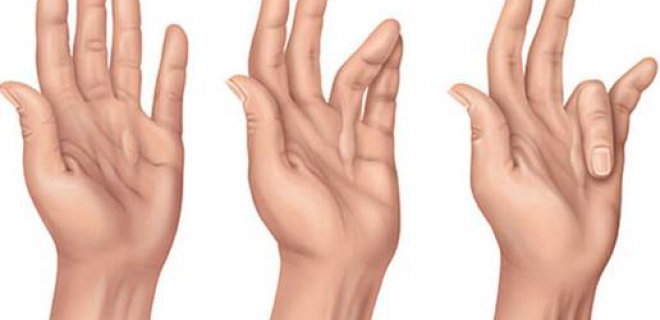
The onset is insidious, starting with painless swelling on the palm, especially at the level of fingers 4 and 5. Increasingly swelling begins to thicken in the form of a band. The flexibility of the fingers is affected as the swelling and hardening of the skin increases. When the patient places the palm on a flat surface, the palm does not touch the ground and takes the form of a dome.
As the disease progresses, it may affect the tendons, adjacent vessels and nerves. It becomes increasingly difficult for the patient to open his finger. Therefore, washing his hands, wearing gloves, clapping and grasping the objects are disrupted.
What are the Symptoms of Dupuytren’s Contracture?
Symptoms of Dupuytren’s contracture begin in the palm and progress to the affected finger. Dupuytren’s contracture, which does not cause any pain, progresses, causing movement limitation of the finger. The insidious onset and progressive disease usually affect the 4th and 5th fingers.
Dupuytren’s contracture, often affecting the middle finger or ring finger, begins with painless swelling at the level of these fingers. The swelling then proceeds by thickening in the form of a band and this swelling restricts the movement of the finger and reduces its flexibility. With the progression of the swelling, the palm is domed and does not touch the ground when placed on a flat surface.
Dupuytren’s contracture, which is a progressive disease, starts to damage tendons, adjacent vessels and nerves.
- Difficulty opening one or more fingers
- Swelling on the palm
- Hardness in the palm
- Hand-held dome (does not touch the ground when placed on a flat surface)
What is Dupuytren’s Contracture Treatment?
There is no need for surgical intervention if the palpable nodules do not cause limitation of movement in the patient. However, a cortisone injection may be performed in appropriate patients to reduce progression. However, this type of treatment must be administered under the supervision of a doctor. If the patient cannot open his / her finger with the progression of the disease, surgical intervention is performed.
In cases of Dupuytren’s contracture diagnosed at an early stage, treatment is started with exercise and physical therapy. The main goal of treatment is to correct the impaired functional capacity and deformity of the hand. Local steroid injection slows progression with anti-inflammatory effect. Also, hand splints and finger contractures are prevented. Shrunken tissues are removed by Dupuytren’s contracture surgery, and in some cases, the skin from other parts of the body is transferred to this area. Physical therapy should be applied after surgery. The disease may recur in 20% of patients.
Muscle Rheumatism (Myalgia)
Myalgia is used for continuous muscle pain. Myalgia may be a precursor to muscle injuries resulting from the excessive and uncontrolled use of muscles.
What is Fibromyalgia Syndrome?
Fibromyalgia syndrome is soft tissue rheumatism that may be prolonged in the musculoskeletal system, causing widespread pain and tenderness in the body. It is sometimes called soft tissue rheumatism or muscle rheumatism.
Why Fibromyalgia Syndrome Occurs?
The exact cause of fibromyalgia syndrome is not known. In the researches, some theories have been put forward. These theories include sleep disorder, pain perception disorder, imbalance of substances called neurotransmitters in the central nervous system, nervous and hormonal system disorders, muscle and muscle dysfunction, and over-functioning of the sympathetic system.
What are the Signs and Symptoms?
A- Musculoskeletal Symptoms: Pain, stiffness, soft tissues can be listed as a feeling of swelling.
B- Non-Musculoskeletal Symptoms: Fatigue, morning stiffness, sleep disturbance, drowsiness, symptoms outside the musculoskeletal system.
C-Accompanying Symptoms: Emotional variability, headache, menstrual pain, diarrhoea and constipation, dry eye symptoms, Raynaud’s phenomenon (colouration of cold in hands and feet)
How is Myalgia Syndrome Diagnosed?
It is not easy to diagnose myalgia; because there is no disease-specific laboratory test. It is necessary to ensure that there is no other disease that can make similar complaints. The patient should be examined carefully by the physician, biochemical and blood tests should be requested if necessary and thyroid function tests should be performed.
In general, fibromyalgia syndrome is diagnosed with long-lasting musculoskeletal pain, fatigue and the presence of vulnerable spots in certain parts of the body. Areas with sensitive points in the body;
What are the Risk Factors for Myalgia?
Gender: It is more common in women than in men.
Age: Most commonly seen in the early and middle adult period. However, it can also be seen in children and the elderly.
Sleep disturbance: How it affects fibromyalgia syndrome is not fully known. It may be accompanied by muscle spasm and restless leg syndrome or sleep apnea syndrome.
Family history: This disease is more common in patients with family history.
Rheumatic diseases: The presence of rheumatic diseases such as rheumatoid arthritis, lupus or ankylosing spondylitis may predispose to fibromyalgia.
How is Myalgia Treated?
As with any disease, informing and educating the patient is very important. The basis of fibromyalgia treatment is drug therapy and physical therapy. The patient should first be told that this disease is a long-term disease and although the pain is continuous, it does not harm the body.
Drug Treatment; Antidepressants, muscle relaxants, painkillers, sleep-regulating drugs, magnesium treatments are often applied.
In physical therapy applications, hot packs, deep heaters and electrical stimulation with pain relief have positive results. Exercise is the most important treatment and prevention method in the disease.
Myopathy
Myopathy is a muscle disease that causes muscle weakness and muscle fibres cannot function for various reasons. In other words, myopathy means any muscle disease that affects muscle tissue.
Causes Myopathy?
Myopathy may occur due to effective diseases, heredity, genetic abnormalities, exposure to toxins, glycogen storage disease, dehydration, and inflammatory diseases.
Subsequent Causes
- Dehydration (dehydration of the body)
- Infectious diseases
- Endocrine disorders
- Myositis (muscle inflammation)
- Neuron disorders
Causes
Myopathy may be a disease that is genetically transmitted to you from the upper generations. Some genetic conditions that result in myopathy include;
- Congenital myopathies (present at birth)
- Muscle glycogen storage disease (including Pompe disease)
- Familial periodic stroke
- Mitochondrial myopathy (abnormalities of cellular components known as mitochondria)
- Muscle dystrophy
Symptoms
Myopathy causes muscular dysfunction due to inflammation or disease and causes some symptoms. Symptoms may also vary from person to person.
Common symptoms of myopathy include;
- Weakness
- Cramps in the joints
- pain
- Paralysis
- Muscle hardening
- Atrophy
- Strain from sitting position, climbing stairs or even combing hair
How is Myopathy Diagnosed?
Diagnosis and treatment of myopathy are performed by a Doctor of Neurosurgery. To diagnose myopathy, blood tests, electromyography (EMG) – tests of nerve signals and muscle function are performed. Muscle biopsy, in which a small muscle sample is surgically removed, may be required for the examination.
How is Myopathy Treated?
Myopathy treatment varies depending on the cause. Myopathy treatment aims to slow down the progression of the disease and alleviate the symptoms. If doctors find that myopathy is caused by an underlying, treatable medical problem, they will first focus on treating it. Other treatments and steps may include:
- Corticosteroids and drug use for immune system treatment
- Vitamin supplements
- Avoiding certain drugs or substances
- Physiotherapy
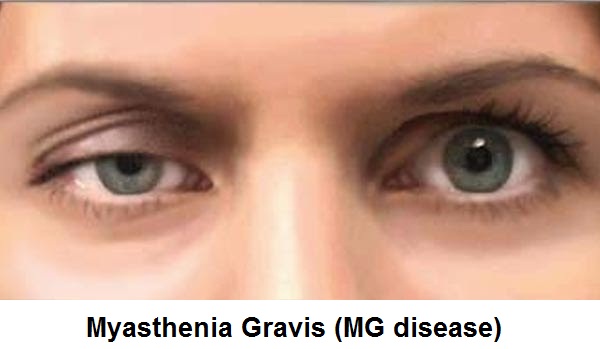
What is Myasthenia Gravis?
Myasthenia gravis is a discomfort caused by the inability of the muscles to communicate. This is because the neurotransmitters involved in muscle communication cannot do their job.
What Causes Myasthenia Gravis?
Myasthenia gravis is caused by the immune system producing antibodies that interfere with the communication of the muscular system. In some cases, the immune system causes a block of chemical stimulants called neurotransmitters. In this case, functional problems occur in the muscular system, which has duties in the basic function of the body.
- The disease may also occur because antibodies produced by the immune system interfere with the functioning of certain proteins affecting the nervous system in the body.
- The disease can also be seen as a result of the functional problem caused by the thymus in the immune system.
- Myasthenia Gravis may cause weakness and headache.
What are the Symptoms of Myasthenia Gravis?
There may be differences in symptoms and severity of the disease. These are as follows.
- Deterioration of eyelids,
- Disorders of expression of muscles in the face
- Difficulty in eating and swallowing,
- Distortion of vocal cords,
- Hard breathing,
- Weakness,
- Headache,
- Having problems in holding objects,
- A slowdown in mobility,
- Difficulty in moving the neck,
- Serious conditions such as visual impairment occur.
Myasthenia gravis is caused by the immune system producing antibodies that interfere with the communication of the muscular system.
How is Myasthenia Gravis Diagnosed?
Myasthenia gravis is the first step that should be taken to the physician to take the symptoms of the person into consideration to be diagnosed. Afterwards, some tests are applied to the patient for definitive diagnosis.
- The patient undergoes extensive physical control by the doctor.
- After a physical examination, a tension test is applied to the patient and muscle movements are examined. In this application, muscle movements are controlled by administering edrophonium chloride to the person.
- After applying a cold compress to the eyelid, changes in the eyelid are examined for a while.
- Blood tests are performed to investigate the formation of different antibodies.
- By connecting the electrode to the person, the muscle conduction status is checked. For this reason, minimum electrical waves are transmitted.
- EMG testing is the most important step in the diagnosis of Myasthenia gravis disease.
- The size of the thymus glands is examined by computed tomography.
- Various breath tests are conducted to determine whether the disease affects the respiratory tract.
The immune system causes the blocking of chemical stimulants called neurotransmitters.
How is Myasthenia Gravis Treated?
In the treatment of myasthenia gravis, various drug applications or surgical operations are applied. Also, different treatment methods can be applied for organs damaged as a result of the disease.
The conditions in which drug treatment is applied are as follows;
- To strengthen nerve and muscle communication, cholinesterase inhibitor is administered. However, various stomach and intestinal diseases can be seen.
- Corticosteroid administration prevents the immune system from producing antibodies. However, this treatment can cause side effects such as weight gain and bone softening.
- Thanks to immunosuppressants, the defence system is suppressed. After this treatment method, problems in kidney and liver functions can be seen.
- Serious conditions such as visual impairment occur.
Surgical conditions are;
The disease affects various organs. Therefore, surgical intervention can be performed on the patient.
- For eye disorders,
- For kidney and liver dysfunction,
- Operations may be performed for bone problems (such as bone resorption).
Myasthenia gravis can become very dangerous for the person. Therefore, treatment should be provided under the supervision of a specialist and never be interrupted. However, with regular treatment, the person can lead a healthy life.
Lambert-Eaton Myasthenic Syndrome
Disease Definition
Lambert-Eaton Myasthenic Syndrome is a presynaptic disease of autoimmune neuromuscular transmission and is often associated with small-cell lung cancer (SCLC) characterized by fluctuating muscle weakness and autonomic dysfunction.
Causes of Lambert-Eaton Myasthenic Syndrome?
In an autoimmune disease, your body’s immune system mistakenly assumes a foreign substance in your own body. Your immune system produces antibodies that attack your body.
In LEMS, your body attacks the nerve endings that control the amount of acetylcholine that your body releases.
In particular, your body attacks a protein called voltage-gated calcium channel (VGCC). VGCC is required for acetylcholine release. You don’t produce enough acetylcholine when the VGCC is attacked, so your muscles won’t work properly.
Many cases of LEMS are associated with lung cancer.
Symptoms
The primary symptoms of LEMS are leg weakness and difficulty walking.
- Weakness in facial muscles
- Involuntary muscle symptoms
- Constipation
- Dry mouth
- Impotence
- Bladder problems
Complications
- Difficulty breathing and swallowing
- infections
- Injuries or coordination problems due to falls
Diagnosis
The diagnosis of LEMS is often delayed because it is rare and can be confused with the more common MG. Because of its association with SCLC, P-LEMS is recognized faster than NP-LEMS.
The major obstacle in the diagnosis of LEMS is the differential diagnosis from other diseases associated with leg weakness.
Electrophysiological
EMG-associated electrophysiological triad:
- Low BKAP amplitudes
- Decrement> 10% in low-frequency nerve stimulation (LFS)
- These are incremental responses in high-frequency nerve stimulation (HFS) or after maximal voluntary contraction.
Single-fiber EMG: Significantly abnormal in LEMS, but not specific to LEMS.
Other reviews
Edrophonium injection (Tensilon test) may temporarily suffer weakness but is not specific for LEMS.
Patients at risk for SCLC (discussable for all LEMS patients with an age of onset> 50 and who are currently or previously smokers) should be examined with lung CT and bronchoscopy should be performed if negative.
Treatment
The treatment of LEMS is personal and partly due to the underlying malignancy.
Symptomatic:
In the presence of metastasis or the use of drugs such as theophylline, which increases seizure risk, low-dose 3,4-DAP may cause seizures. The use of 3,4-DAP is contraindicated in patients with seizures.
Immunomodulation
Intravenous immunoglobulin (IVIG) or plasmapheresis
Treatment of Underlying Malignancy
Chemotherapy and radiotherapy
Botulism (Botulismus)
Botulism is an extremely dangerous or even deadly food poisoning. The disease is caused by a bacterium called Clostridium botulinum. This bacterium is abundant in nature and sometimes enters into food and causes botulism. Bacteria produce offspring called spores that last for years. These spores do not die by boiling. Reproduces in an oxygen-free environment. It can easily multiply in foods such as canned honey and produce poison and cause disease. Botulism poison paralyzes, is a very powerful poison. A very small proportion of this poison is also used for treatment.
What Causes Botulism?
The disease is caused by the ingestion of the toxin produced by Clostridium botulinum. Even a small amount of this poison is enough to kill people.
Botulism Appears as follows:
Foods: If the bacterium itself or the toxin produced by the bacteria is transmitted to the food, the disease occurs in those who eat it. The most common cause of botulism through food is:
- Homemade canned food,
- Sausage, salami, sausage and meat products,
- Sea products,
- Vegetable preserves, (especially alkali vegetable preserves such as peas, beans),
If babies swallow the spores of the bacterium Clostridium botulinum, bacteria can grow in the baby intestine, causing botulism. The most common source of this type of botulism that is not seen in children and adults is eating soil and eating honey.
What are the symptoms of botulism?
Complaints usually occur within hours, at the latest after 36 hours. The first complaint occurs in the eyes and eyelids. Falling eyelids and double vision are the first complaints. The disease then paralyzes the entire body by spreading downward and paralyzing the respiratory muscles, leading to death.
- Falling eyelids,
- Double vision, blurred vision,
- Dizziness, weakness,
- Swallowing difficulty,
- Drying in mouth,
- Throat ache,
- Difficulty speaking, don’t talk like a drunk,
- Incontinence of head and neck,
- Difficult to breathe,
Symptoms in infants:
- Falling eyelids,
- Incontinence,
- Fatigue tends to fall asleep,
- Nutritional difficulty,
- Muscle laxity,
- Constipation swelling in the abdomen,
- Weak crying occurs.
How is Botulism Diagnosed?
The patient’s complaints and examination findings are helpful in the diagnosis. The doctor should explain in detail how the disease develops. Blood, faeces and stomach contents can be evaluated for the toxin. If you have suspicious food can be analyzed. Wound culture can be performed in wound-induced botulism.
Suspecting Botulism:
Blood tests, MRI examination, whether there is the intracranial formation that may cause this condition, Cerebrospinal fluid examination, can be done.
Botulism Treatment
The deadly effect of botulism is respiratory muscle paralysis and respiratory arrest. Botulism is extremely dangerous and deadly food poisoning. Even in the slightest doubt, a doctor should be consulted. In the treatment of botulism, the patient is given respiratory support, oxygen is given and taken to intensive care. If necessary, connect to the auxiliary breathing apparatus. Since it has difficulty swallowing, it is fed by tube.
Botulism antitoxin: The main point of treatment. Antitoxin stops the progression of paralysis in early cases. It allows treatment to be successful and shorter complaints. Does not return paralyzed parts.
Excretion of toxin: for excretion of toxin that has entered the body but has not yet been absorbed:
- Diarrhoea drugs,
- Stretching the stomach contents,
- Vomiting drugs,
If the wound is caused by extensive cleaning of the wound and antibiotic administration stops the further progression of the disease.
Protection from Botulism
Botulism toxin loses its effect by cooking at high temperature. It is important not to eat or destroy suspicious foods. To avoid botulism:
- Honey should not be given to babies under 2 years of age,
- Garlic, spices, pepper and so on. The oils should be stored in the refrigerator.
- Don’t taste bad food,
- Do not take or use canned food with a swollen lid,
- Cook potatoes without wrapping with foil, if you wrapped in foil, consume while hot, do not put in the closet,
- Soak the canned food in boiling water for 10 – 20 minutes before consuming,
- Pay attention to hygiene when canning,
- Do not make your wound dressing, even in the slightest injury to the health centre, see a doctor,
Double vision and low eyelid are the most important first signs of botulism. If you suspect botulism, seek medical advice immediately.
Myositis
What is Myositis?
Polymyositis and dermatomyositis are connective tissue diseases characterized by muscle inflammation. An idiopathic inflammatory myopathy is a group of chronic, autoimmune conditions that primarily affect the proximal muscles.
Although dermatomyositis affects the skin and muscles, it can also affect other parts of the body such as joints, oesophagus, lungs and heart. Both polymyositis and dermatomyositis have an autoimmune basis. Polymyositis produces muscle weakness. Although a few patients complain of pain or cramping, it is not painful. Polymyositis is a muscle disease which has the characteristic of inflammation of muscle fibres.
Myositis Types
There are several types of myositis that affect muscles:
Polymyositis – affects many different muscles, especially the muscles of the shoulders, hips and thighs; It is more common in women and tends to affect people aged 30 to 60 years.
Dermatomyositis – affects muscles but causes rashes; More common in women Affects adults and children
Post-infectious reactive myositis – can get after some viral infections and cause inflammation of the muscles; This type of myositis is usually mild and passes untreated.
Symptoms of Polymyositis
Polymyositis affects many different muscles, especially the neck, shoulders, back, hips and thighs.
Symptoms include:
- Muscle Weakness
- Painful muscles
- Overstrain
- Usually, you don’t feel well
Other more general symptoms, including joint pain, and sometimes swelling and shortness of breath may be present. Muscle weakness can vary from week to week or month to month but tends to get worse without treatment.
Symptoms of Dermatomyositis
Dermatomyositis also affects muscles and the symptoms are similar to those of polymyositis (see above). However, there are also significant rashes. A red or purple rash occurs on the face (eyelids, nose and cheeks), upper chest, elbows, knees and joints before the appearance of muscle symptoms. The rash may be itchy or painful and may also develop hard tubers under the skin called calcinosis.
Diagnosis of Myositis
Your doctor will ask you about your symptoms and examine you. If they think it may be a myositis, you should take some tests to help eliminate other conditions with similar symptoms.
Blood tests – to check if your blood enzymes and antibody levels are elevated
Muscle or skin biopsy – a small sample of muscle tissue and skin can be taken so that it can be examined for inflammation, damage and other abnormalities
Magnetic resonance imaging (MRI) scans – modern scanners can accurately determine the extent of inflammatory changes in muscles and distinguish real areas of inflammation where muscle fibres are replaced by fat or fibrous tissue
Electromyography (EMG) – a small needle-shaped electrode is inserted into the scalp and intramuscularly using local anaesthesia to record electrical signals from nerve endings in the muscles; An abnormal form of electrical activity may indicate that you have polymyositis or dermatomyositis
If you have serious symptoms of myositis such as severe muscle pain and weakness, you should be very careful about exercise. Most experts do not recommend exercising during this time. Once the condition is controlled, a soft exercise program can be initiated and gradually increased upon the advice of a physiotherapist.
Treatment
How treatment is performed;
Immunosuppressive drugs are used. Cortisone treatment is the first drug of choice. Cortisone does is reduced while immunosuppressive drugs are added to prevent recurrence of the disease. Rituximab and IVIG treatment are given in resistant cases.
Secondly, and very importantly, to strengthen the muscles, appropriate exercises should be performed at an early stage. Physiotherapists who are experts in this field should be assisted and the patient should be re-rehabilitated and raised.