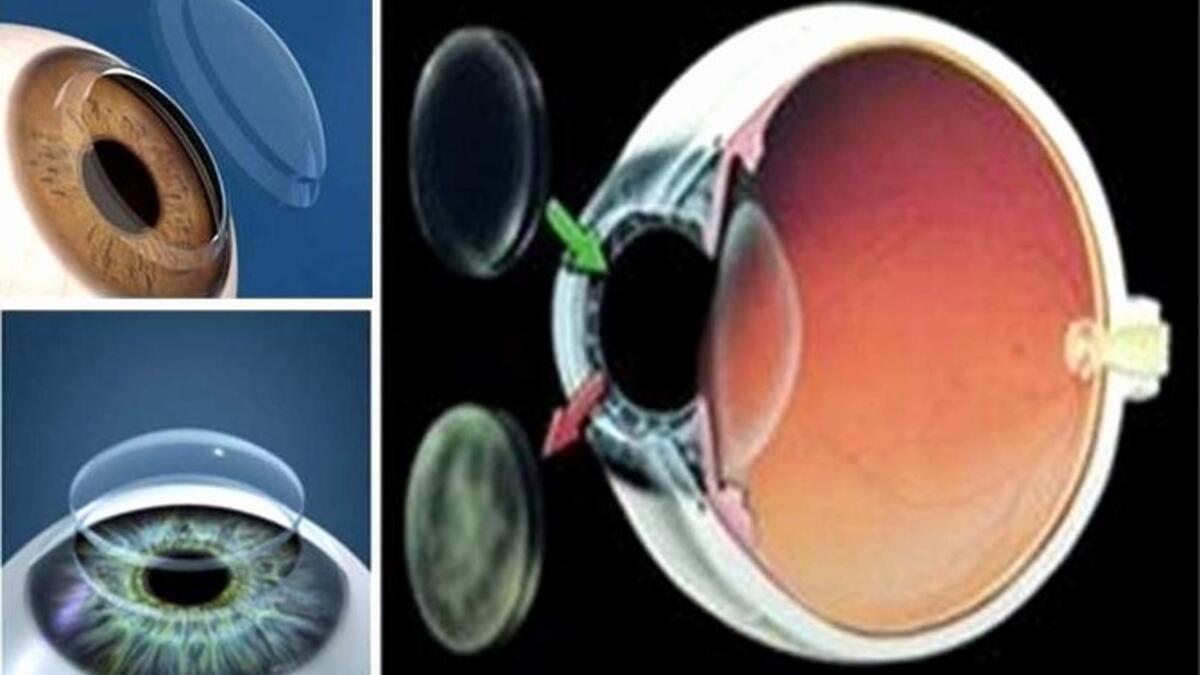
Laser Cataract Surgery
It has been used in cataract surgery for the last 2-3 years. It is used in some stages of the surgery and then continued with the phaco method. The fact that the standards have not been fully fulfilled limits the use of 5-minute vacuum in the eye during surgery and the risk of frequent bleeding and bleeding in postoperative patients.
What is a cataract, how is it treated?
The cataract is an opaque appearance by losing the transparency of the lens in the anterior-middle part of our eye. In other words, the transparent lens is frosted glass.
What are the causes of cataracts?
- Ageing: the most important cause of cataracts is ageing. A cataract is detected in the majority of people of older ages.
- It is more common in family members with cataracts.
- Metabolic diseases: cataracts are common, especially in diabetes.
- Trauma (blunt and penetrating eye injuries)
- Long-term use of cortisone drugs
- Other eye diseases (eye infections, vascular diseases, etc.)
- Exposure to sunlight
- It is considered one of the most important causes of cataract formation.
What are the symptoms of cataracts?
Complaints of patients may vary depending on the type of cataract. The most important symptom is the decreased vision. Especially when the other eye is closed. At night, light disturbance, difficulty in reading, sometimes in the dark, sometimes in the sunlight is seen to decrease vision. In some cataracts, distant vision deteriorates due to false myopia and near vision improves. Then the close vision is impaired. Fading and yellowing of the colours is another finding.
How is cataract treated?
The only treatment of cataract is surgery. There is no drug treatment. Used vitamin drugs and so on. No contribution of drugs to the treatment and prevention of cataract development was found.
Refractive Surgery (Excimer Laser)
The cornea is a transparent layer in the form of a watch glass at the forefront of the eye. If the rays penetrating the eye due to defects in the shape of the corneal layer or eyeball cannot focus sharply on the retinal layer, defects in the focusing power of the eye are called refractive defects (refractive defects). Three major refractive errors; myopia, hyperopia and astigmatism.
Myopia: The eye can not focus on objects beyond a certain distance is called myopia. It is popularly known as the inability to see far. Generally, the anterior-posterior diameter of the eyeball is longer than normal. Therefore, the incoming rays fall to the front of the retina and the lens cannot reduce its curvature beyond a certain limit.
Hyperopia: Eyeball is usually shorter than normal. This causes nearby objects not to focus. Often, hyperopia, such as myopia, is a factor of inheritance.
Astigmatism: Astigmatism is usually caused by irregularity or distortion of the cornea. In astigmatism, the slope of the cornea is greater in one direction.
EXCIMER LASER
Laser technology has been used for many years in the treatment of eye diseases.
Different laser technologies are used for different eye diseases.
Commonly known as “eyeglass relief” surgery or “eye drawing” operations are laser eye treatments using excimer laser.
Who Can Treat Excimer Laser?
- 18 years of age,
- Over 0.50 eye defects have not changed in the last two years,
- Myopia up to -10 degrees,
- Astigmatism up to -6 degrees, hypermetropia up to +6 degrees,
- Corneal tissue thick enough people
Excimer Laser Types
LASIK, LASEK or PRK technique is used to correct visual disturbances with the excimer laser.
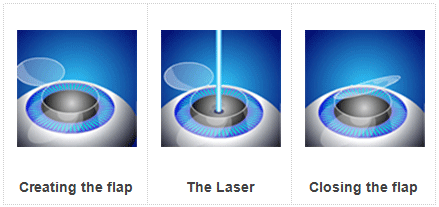
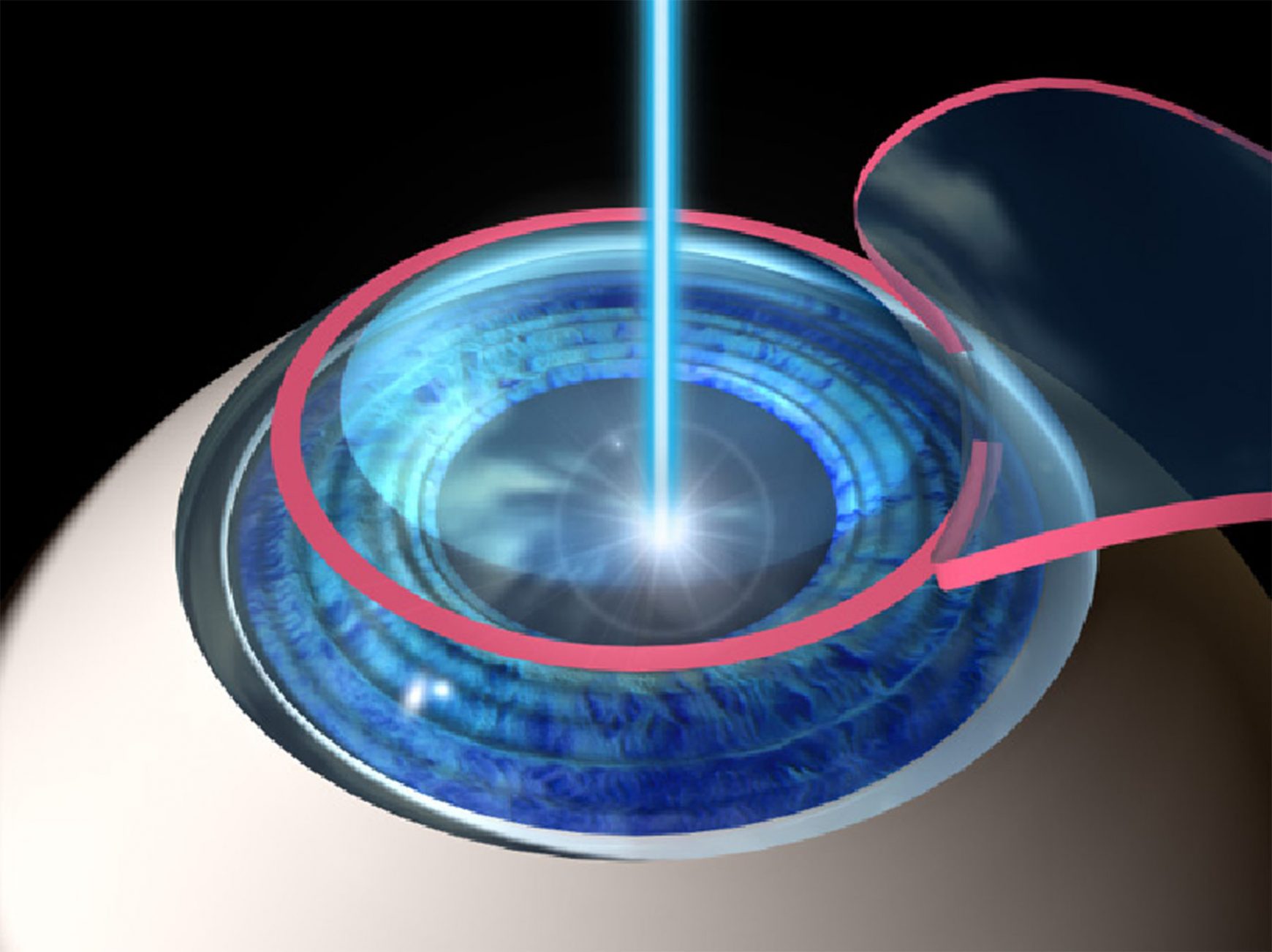
What is LASIK?
In the LASIK method, the corneal layer is permanently reshaped with an excimer laser to eliminate the existing refractive error.
- Lasik corrects myopia, hyperopia and astigmatism.
- In the post-Lasik number, there is no return or very low numbers.
- After Lasik, the number becomes more stable.
- Both eyes can be operated at the same time.
- One day can occur without hospitalization.
- Patients can return to their daily activities within 24 hours.
Why LASIK?
The total duration of treatment is approximately 15 minutes. The duration of the laser is only 15-20 seconds.
- Lasik is the most preferred laser surgery in the world.
- There is no need to close the eyes after treatment or stay in the hospital.
- Visual acuity starts to increase a few hours after the operation.
- The laser is applied to the anterior part of the eye, so there is no external anatomical change in your eye.
Pre-LASIK Assessment
If you have decided for LASIK treatment, you should first examine whether you are a suitable candidate by a detailed examination.
LASIK surgery is a laser procedure performed with drop anaesthesia, which lasts for 15 minutes and the results are very pleasing, but it is very important for the patients who have decided to undergo LASIK treatment that they understand the risks and benefits of the operation very clearly.
LASEK
In the LASEK technique, the epithelial layer, which is the top cover of the cornea layer, is separated and removed with the help of alcohol. The epithelial layer is re-implanted after laser treatment to correct the refractive error. The LASEK method is used for LASIK treatment, especially in thin corneas with insufficient thickness. It is preferred in people who are likely to experience problems with it. The recovery period after LASEK takes a little longer. Although it varies from person to person, the sensation of stinging in the eye continues for the first 1-2 days after LASEK and vision may take between 4 days and 1 week.
PRK
In PRK method, myopia, hyperopia or astigmatism are corrected with excimer laser after removing a thinner layer from the transparent surface of the eye. In this method, the removed film is not replaced. As in Lasik, anaesthesia drops are dripped before the procedure and no pain or pain is felt during the procedure.
No Touch Laser Technique (Trans PRK)
PRK is a new type of surgical technique. In this method, as in PRK, there is no need to remove the valve from the corneal surface, the difference from PRK is removed by laser (Femtosecond) method, not by the epithelial knife on the corneal surface.
Laser application is performed quickly under the removed epithelium and the operation is terminated. It is preferred in patients with thin corneas that are not suitable for Lasik technique, and severe eye pain may occur during the first 2 days after the operation.
A soft contact lens is applied to the eye for the bandage to relieve pain severity and to improve healing quickly.
Smile Laser Technique
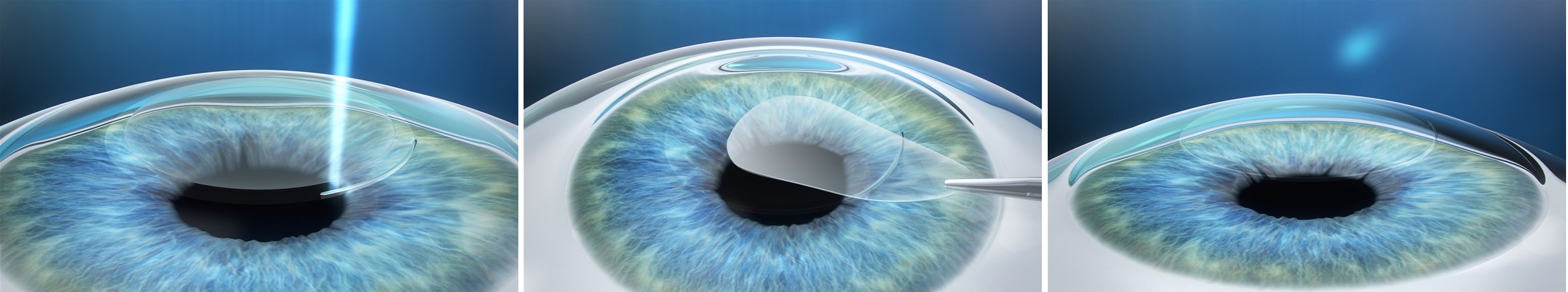
As an alternative to the LASIK technique, a new laser procedure called Smile has been developed in recent years. Smile name of this method, which was approved by FDA in 2016 for use in the USA, is derived from the words Small incision Lenticule Extraction.
In this laser surgery method, the surgeon uses a Femtosecond Laser to create a small lens-shaped tissue (Lenticle) in the cornea. Then, with the same laser, a very small aperture on the outer surface of the cornea is made in the form of an arc less than 4mm and the surgeon removes and discards the Lenticulum from this incision, and when the small Lenticulum is removed, the shape of the cornea changes and distant vision is corrected.
The small incision in the cornea will heal within a few days without a seam and sharp vision occurs very quickly. Smile laser eye surgery can correct myopia up to -10.00 dioptres, candidates must be at least 22 years old, have maximum astigmatism of -0.50d and prescription glasses should be stable for at least 12 months.
Smile Lasik technique is a form of treatment performed without the need to create a corneal flap. Therefore, there is less risk of dry eye symptoms after smile compared to LASIK.
Laser Will Attention Patients
Before treatment
There is no harm in eating the patient on the day of treatment.
Patient only;
- Do not make eye makeup,
- Don’t use perfume,
- No drink blood thinners.
Treatment order
When the patient enters the laser room, he is asked to lie on his back on the laser bed. The eye is cleaned with a baticon and a sterile drape is covered, then the eyelids are spaced with a specially designed apparatus to prevent blinking during the treatment. Laser treatment lasts about 4-5 minutes for each eye, no pain or pain is felt. The patient leaves the laser chamber without bandaging his eyes after the treatment is finished.
First 24 hours after treatment
After the laser treatment is completed, the patient is examined postoperatively. The patient can leave the hospital after this control. First day; blurred vision and stinging in the eyes for 5-6 hours, burning and watering are normal. The use of medication should be observed in the manner prescribed by the doctor. If the headache is felt after laser, a painkiller without blood thinner can be taken. On the day of surgery can not drive and can not go to work .
Dusty environment should be avoided, the eye treated during the first 24 hours should not rub, itch, hands, face wash and bath should not be done. In the first days, soap and shampoo should be avoided. The next day after the operation, there are no side effects that limit the social and work life. If a wrinkle is detected in the transparent area on the surface of the eye, or if a reaction under the flap occurs, a flush of gold may be required.
Contact Lenses
Contact lenses are used for correcting visual defects such as myopia, hyperopia, astigmatism and presbyopia, changing eye colour or some corneal diseases.
Far from myopia, close to hyperopia can not see clearly. Astigmatism is to see skewed and broken due to the drop of light coming into the eye to multiple points in the retina. Astigmatism may be due to the cornea (the transparent layer in front of the coloured part of the eye) or the natural lens inside the eye. Presbyopia is a vision problem due to the decrease in adaptability after 40 years of age.
Although the most common use of contact lenses is the correction of refractive defects, it can also be used for cosmetic purposes to change eye colour or for the treatment of corneal injuries. Different contact lenses have been developed for these applications.
The correct contact lens is prescribed as a result of a detailed eye examination for the patient’s needs.
Contact a doctor before selecting contact lenses
The choice of contact lenses you want in your ophthalmologist’s eye examination. It is evaluated whether the patient is suitable for contact lens use. The exam determines the lens type, grade, base curve and lens.
Lens application is performed for the first time with the person wearing contact lenses and the ophthalmologist evaluates the movement, balance and visual acuity of the lens. Lens receiver, take the contact lens there.
Contact Lens Types and Uses
Spherical Contact lens: Contact lens that does not have astigmatism correction and corrects refraction defects such as myopia or hyperopia
Toric Contact lens: Contact lens with astigmatic refractive error correction
Multifocal Contact lens: A soft contact lens that corrects the vision problem of relatives after 40 years of age.
Gas-permeable Contact lens: Hard lens used in cases of high astigmatism or keratoconus due to the cornea (a disease where the cornea is progressively thinner and tapering forward)
Hybrid Contact lens: The lens is made of hard central and soft material around the cornea due to high astigmatism or keratoconus disease.
Colour Contact lens: Soft contact lens that cosmetics change eye colour when worn
Therapeutic Contact lens: Soft contact lens used to treat wounds on the corneal surface
Features of Contact Lenses
- Provides a wider field of view than glasses.
- Blocking the edges on the edges.
- It provides better depth perception than glasses.
- Provides a natural exterior appearance.
- Wearing glasses, misting, and pain due to frame contact is not difficult to wear.
- Colour lens designed for cosmetic eye colours.
- Practical and safe use possibilities in mobile activities such as sports.
The contact lenses are shaped to rest on the cornea. The lens that is suitable for the eye stops in a well-centred manner. The lens for the circulation of tears is to move slightly.
After wearing contact lenses, the user should be able to see clearly and comfortably and should not feel the presence of the lens. Change of concept after the eye should not change.
Cautions When Using a Lens
Although contact lenses can be used monthly, it is recommended not to comply with contact lenses.
It is wrong to go into the sea or pool with contact lenses. If contact lenses are used incorrectly, it will cause germs to adhere to the cornea. Causes serious eye infections.
If red-eye or stinging sensation occurs while wearing contact lenses, the user should immediately remove the lens and consult a doctor.
Corneal Transplantation
The transparent layer in front of the iris layer, the coloured part of the eye, is called the cornea. After the first rays of the eye pass through this tissue, it reaches the nerve layer called retina and vision occurs.
The transparency or regular shape of the cornea, therefore, plays an important role in vision. If the cornea loses its transparency (hereditary diseases such as dystrophy of the cornea, persistent corneal oedema after cataract surgery, etc.) or deformed (progressive thinning and erecting of the cornea such as keratoconus), the patient cannot see clearly.
In such cases, the cornea can be replaced with another healthy corneal tissue to restore the vision. The tissue in this transplant is healthy corneal tissue taken from a person who has lost their lives and the process is called corneal transplantation.
Corneal transplantation can be performed with full-layer corneal tissue or transplantation of only the upper layer or the lower layer of the cornea.
One of the features of the cornea that makes it transparent is that it is vein-free. The absence of veins in the tissue provides an important advantage in tissue transplants. Because it is not possible for the cells that cause tissue rejection to reach foreign tissue.
When we consider all transplant operations, corneal transplants are more successful than other transplants because of this feature.
Steps of Full-Corneal Transplant (Penetrating Keratoplasty) Surgery
- Disinfect the eye and its surroundings under local or general anaesthesia and cover with a sterile drape.
- The centre of the cornea is marked.
- Make a circular full-thickness incision with a diameter of 7-7.5 mm in the centre of the cornea with a vacuum tool (trepan) containing a round blade and remove the centre of the cornea.
- The donor cornea is prepared with a vacuum tool with a circular knife (punch) to suit the recipient bed.
- It is sutured to the receiving bed with different stitch techniques (16 single stitches, 16 single stitches with continuous stitches, continuous double stitches, etc.).
- Antibiotic medication is applied to the eye and the procedure is ended.
The duration of the operation is approximately 30-40 minutes. If there are other attempts at the same time, the operation time may be prolonged.
After Full Layer Corneal Transplantation
Complaints such as stinging and watering may occur after a few weeks. The protective bandage is used on the day of surgery.
The visual level may not increase immediately. Postoperative antibiotic and cortisone eye drops are used according to the physician’s recommendation. The first control is performed on the first postoperative day. Thereafter, a check is carried out every month for the first week and the first year. Stitches are usually taken after 1 year.
Complications During Full-thickness Corneal Transplantation
Expulsive haemorrhage: It is difficult to control as a result of the accumulation of blood in the choroid which is the vascular tissue of the eye. This is very rare (0.45-1.08%). It is not possible to predict in advance and if it happens, it may result in loss of an eye.
Astigmatism: Astigmatism is common after corneal transplantation. The sutures placed with tissue healing change these astigmatism values over time. Astigmatism can be removed with stitching, re-stitching, loosening incisions or LASIK.
Increased intraocular pressure (glaucoma): It can be seen in the early or late period. The early intraocular pressure increase is rapidly controlled with medications. The increase in intraocular pressure in the late period is usually due to the drops with cortisone used. In this case, drugs that lower intraocular pressure should be used.
Infection: Serious infections can be seen after intraocular surgery, although very rarely. This is an important condition, it requires early intervention.
Tissue rejection: It can be seen especially in patients with vascularization of the cornea for other reasons. In such cases, special needles are injected into the eye to prevent rejection of the tissue with drops and drugs.
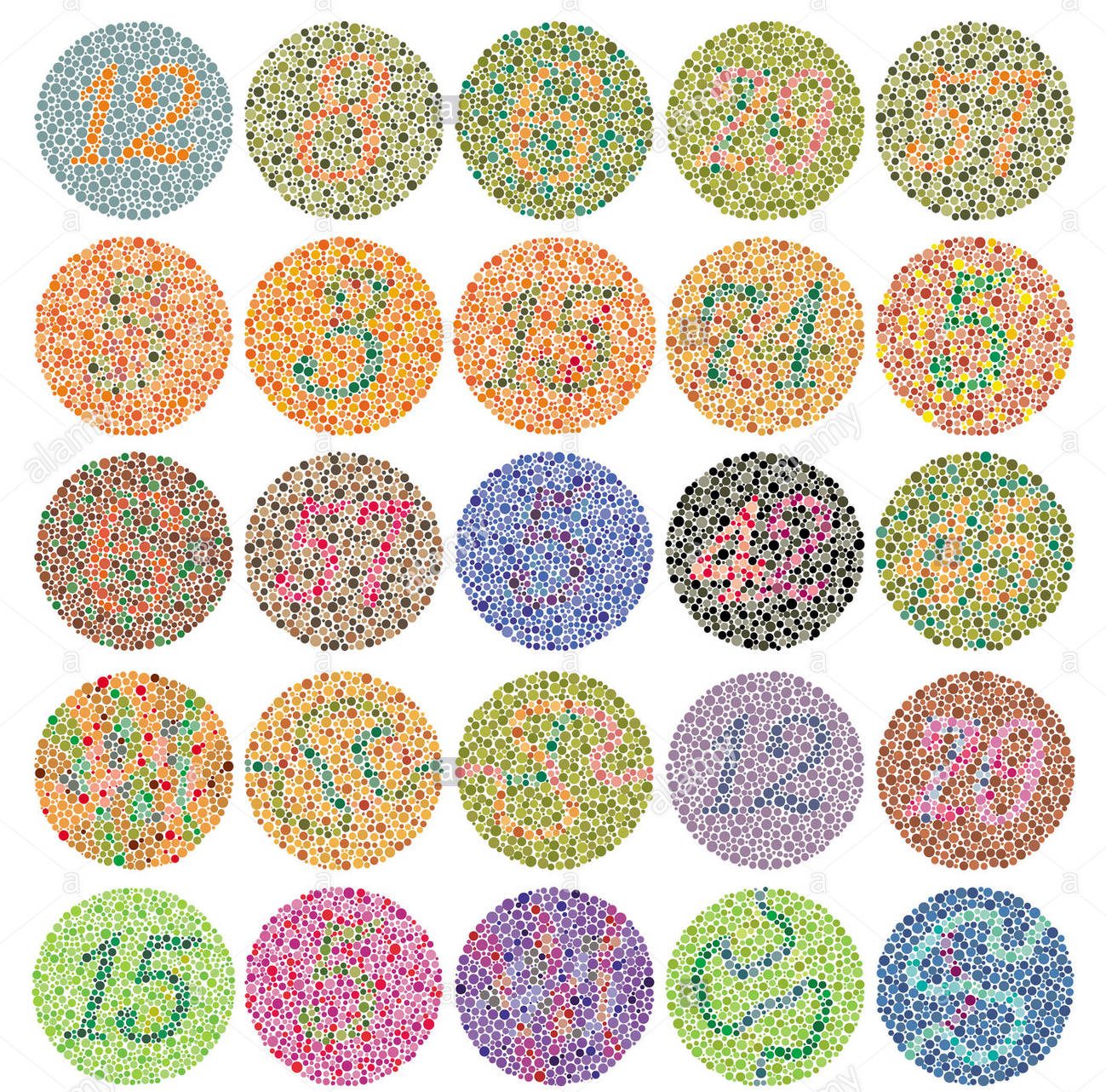
Colour Blindness
Colour blindness is a weakness in the sense of colour and difficulty in distinguishing between blue and yellow or green and red.
It is an inherited condition and affects men more than women.
Symptoms and Signs of Color Blindness
There is a common belief that colour blind people cannot see any colour and see the world in shades of grey. However, this is not true.
Colour blind people see colours, but because they see some colours pale, they can mix colours.
This tests tell you whether you are colour blind or not.
What Causes Color Blindness?
There are photoreceptors called “rod” and “cone” in the layer of the eye called retina. The cones are responsible for seeing the colour. In patients with colour blindness, some cones are inherited.
Can Color Blindness Be Treated?
In a study conducted in the USA in 2009, colour blindness in monkeys was corrected by gene therapy. However, gene therapy cannot be performed in humans yet.
Colour-blind people will experience difficulties in performing professions such as graphic design, fine electronic work and surgery. But in other professions and daily life, colour blind people do not have much difficulty.
Color Blind Special Contact Lenses & Glasses
Colour contact lenses and glasses for colour blind are available. Your ophthalmologist will check you different colours from the trial set of these contact lenses and glasses. The colour of the contact lens or eyeglasses is determined by which colour you can distinguish better. Then you can start using this contact lens and glasses.
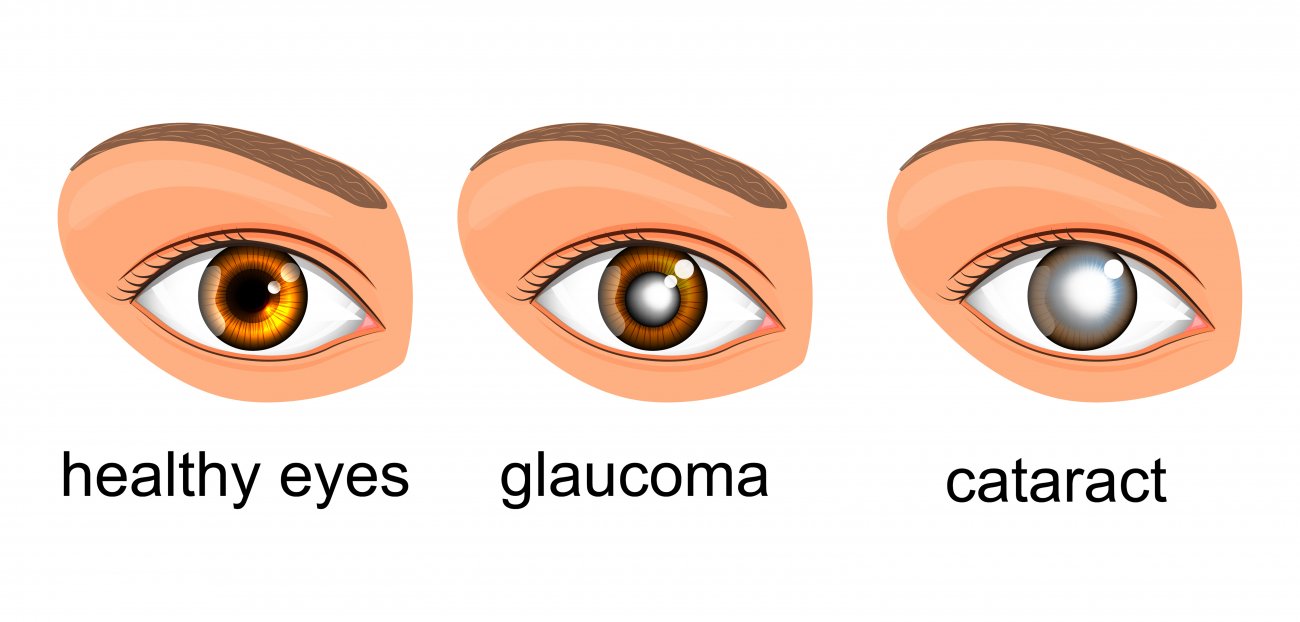
Glaucoma
A glaucoma is a group of eye diseases that cause progressive damage to the optic nerve.
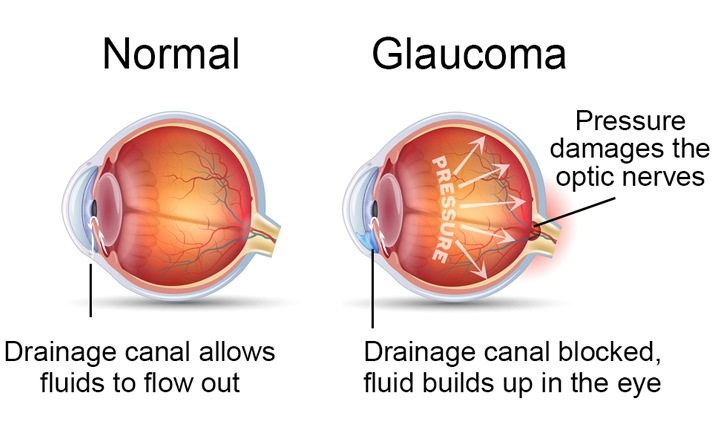
In glaucoma, also known as “Eye Blood Pressure”, the visual nerve is damaged because of the high intraocular pressure for a long time. The visual nerve goes out of the eye to the brain and plays a role in the transmission of information from the eye to the brain.
Glaucoma can lead to slow progressive and irreversible visual nerve damage and consequently loss of vision, leading to blindness.
There is no complete treatment for glaucoma and it is not possible to restore vision loss; however, with early diagnosis and correct treatment, disease progression can be slowed and delayed.
Intraocular Pressure – IOP (Eye Pressure)
As the only changeable risk factor for glaucoma is high IOP, patients often want to know what range of intraocular pressure is considered normal. Unfortunately, the “normal” value varies from person to person, and the value that is normal for one person may be high for another. Even people with normal IOP may develop glaucoma.
Normally acceptable values for an individual are tolerable levels without damaging the visual nerve.
Therefore, regular and comprehensive examination of dilated eyes is essential for the diagnosis and treatment of the disease.
Types of Glaucoma
There are two main types of glaucoma: primary open-angle glaucoma and closed-angle glaucoma.
Primary open-angle glaucoma is the most common type of glaucoma and accounts for almost 90% of cases.
Open-Angle Glaucoma
Its, also known as wide-angle glaucoma, is caused by very slow fluid flow in the anterior part of the eye and consequently increased intraocular pressure (IOP). Open-angle glaucoma often does not show any symptoms, so the symptoms are usually not detected until the disease reaches an advanced stage.
Symptoms:
- Patients may not notice any visual problems until they lose 40% of their visual function.
- When the disease progresses, peripheral vision (vision on the sides of the visual field) may occur, such as tunnel vision or eye points.
Closed Angle Glaucoma
Closed-angle glaucoma, also known as acute or narrow-angle glaucoma, is caused by the difficulty in the drainage of the eye fluid and the sudden increase in eye pressure due to the narrower angle between iris and cornea. Closed-angle glaucoma is more common in hyperopia.
Symptoms
- Headache
- Eye pain
- Nausea
- Formation of halos around night lights
- Blurred vision
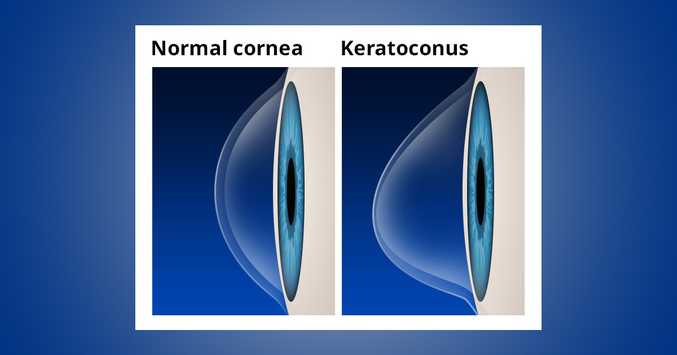
Keratoconus
Keratoconus is the conical tapering of the normally rounded cornea (the transparent layer of the eye) forward. It is a progressive and visually impaired disease, usually begins in adolescence.
What Causes Keratoconus?
The cause of this disease is the imbalance of enzymes in the cornea. As a result, so-called “free radicals” cause oxidative damage to the cornea. Thus, the cornea weakens and waits forwards.
Genetic predisposition applies to this disease. Therefore, more than one keratoconus patients in the same family are frequently encountered.
Other reasons include; ultraviolet rays of the sun, excessive eye rubbing, use of contact lenses that do not fit the eye well, and chronic eye irritation.
What are the symptoms of Keratoconus?
Keratoconus disease usually affects both eyes and can cause very different problems between the two eyes. Symptoms may vary differently in each eye and vary over time. Early-stage, keratoconus symptoms;
- The slight blur of vision
- The slight distortion of vision due to curled or wavy lines
- Sensitivity to light and glare
- Redness or swelling of the eye.
In advanced stages, symptoms become more pronounced. Some of the symptoms of advanced keratoconus are;
- Impaired vision and increased blurred vision
- Increased myopic or astigmatism findings and need for glasses
- Corneal protrusion because contact lenses do not fit the eye or cause discomfort.
The transition from keratoconus to early-stage usually takes years. But in some people, the deterioration occurs more quickly. The cornea may swell suddenly and permanent hardening of the cornea, called scarring, may begin.
Cornea; When this scar tissue is called scar, it loses its softness and clarity. As a result, vision becomes more distorted and blurred.
How is Keratoconus Diagnosed?
Keratoconus can be diagnosed by a routine eye examination. Your ophthalmologist examines the cornea and measures its curvature. This examination helps to determine if there is any change in the shape of the cornea. Your ophthalmologist can map the corneal surface using a special computer. These detailed maps clearly show the condition of the corneal surface.
How is Keratoconus Treatment Done?
Treatment of keratoconus depends on the symptoms and stage of the disease. In the early stages when the symptoms are mild, your eyesight can be corrected with glasses. You may then need to use special hard contact lenses to help focus the image correctly.
There are other methods used to treat keratoconus. Surgically, a small curved device is inserted into the cornea to correct the curvature of the cornea. Your ophthalmologist uses a special UV light and eye drops to strengthen the cornea. Doing so may cause the cornea to flatten or harden, helping to prevent it from becoming more fluffy.
When symptoms are severe, your doctor may recommend corneal transplantation. With eye transplants, your doctor will replace the whole or some of the diseased cornea with healthy donor corneal tissue.
Uveitis
What is Uveitis?
A sheath consisting of 3 layers surrounds the gel-like substance in the middle of the eye, which is similar in structure to a ball. The outermost part is the white part called the sclera, the inner part is called the retina, and the part that allows us to see is the uvea in the middle. Uveitis is called uveitis. Uvea contains veins that feed the eye. The inflammation here affects all tissues of the eye. This situation causes serious situations that threaten vision.
What are the Symptoms and Causes of Uveitis?
Sensitivity to light, pain, redness in the eye, decreased vision are the most important symptoms. In most cases, the cause is not found in some patients; viruses, fungi, parasites and other parts of the body, such as Arthritis, Behçet’s Disease, Infections (bacteria, viruses, parasites or fungi), eye trauma, immune system diseases, rheumatic diseases, ulcerative colitis is known to cause uveitis. The cause of uveitis cannot be found in 30-40 per cent of patients. So it is necessary to investigate various assays and diseases.
How is Uveitis Diagnosed?
Regardless of its severity, uveitis is an urgent disease and needs to be recognized immediately. When late, the disease progresses and may cause permanent side effects such as deformities of the pupil, cataracts and increased eye pressure.
Some diseases can be diagnosed immediately because of their very typical appearance. Even in this case, if the posterior part of the eye is involved, advanced techniques such as angiography, ultrasonography, ERG may be necessary to understand the extent to which vision is threatened and to monitor the effectiveness of treatment. When the symptoms begin, you should see an ophthalmologist; joint treatment with internal medicine and rheumatology unit may be required after treatment has started.
How is Uveitis Treatment?
Especially, drops containing steroids and pupil-enlarging drugs are frequently used. Inflammation deeper in the eye may require the use of systemic drugs. Various complications such as glaucoma, cataract, neovascularization (formation of new vessels) may develop.
Retinal Diseases
The retina is the innermost layer behind our eye. There are visual cells (cone and bacillus) on it. 95% of the visual event occurs at the yellow spot (macula) in the centre of the retina. Especially diabetic retinopathy and macular degeneration can cause damage at the yellow spot.
Diagnostic methods
- Eye angioma (FFA and ICG)
- OCT
Treatments Applied in Retinal Section
- Treatment of retinal tears and detachment,
- Trauma surgery – intraocular foreign body extraction,
- Intraocular inflammation and uveitis treatment.
Diabetic Eye Disease
Diabetes is a systemic disease that causes the most damage to the eye. It is the most important cause of blindness in society. It does the most damage to the retinal layer (diabetic retinopathy). However, it facilitates the formation of a cataract, dry eye and glaucoma. Modern instruments such as eye angiography (FFA) and optical coherence tomography (OCT) are used to diagnose diabetic retinopathy. It can be treated with timely intervention and blindness is largely prevented.
Treatment of; Argon laser treatment is the most important treatment. In cases where oedema develops in the visual centre, intraocular drug applications are performed. Vitreoretinal surgery is performed in the future.
Macular Degeneration (Yellow Dot Disease)
Age-related damage at the yellow spot is the most common cause of blindness in people over the age of.45. The vascular ball that occurs under the macula can be treated with special drug application into the eye. Before treatment, eye angiography (FFA, ICGA) and OCT should determine the type of disease, size and stage of the vascular ball. Photodynamic Therapy (PDT) can also be performed in the required patients.
Vitreoretinal Surgery (Vitrectomy Surgery)
It helps patients regain their vision, especially in advanced diabetes. It is made by drilling 3 holes with a diameter of approximately 1 mm into the chamber. Postoperative fluid, gas or silicone is placed in the eye depending on the condition of the disease. Most of the time, stitches are not used.
Eyelid Disorders
Your eyelids help protect your eyes. When you blink, your eyelids spread moisture over your eyes. Blinking also helps move dirt or other particles off the surface of the eye. Closing your eyelids when something is coming towards your eyes can protect them from injuries. Like most other parts of your body, your eyelids can get infected, inflamed or even develop cancer. There are also specific eyelid problems, including:
- Eyelids that turn in or out.
- Eyelids that droop.
- Abnormal blinking or twitching.
Treatment of eyelid problems depends on the cause.
Introduction
Many disorders can affect the eyelids. Like most other parts of your body, your eyelids can get infected, inflamed or even develop cancer. Eyelid disorders can affect your vision and your daily life. This health information explains eyelid disorders. It also discusses the importance of the eyelids, symptoms of common eyelid disorders and treatment options.
The Eyelids
Its keep the eyes moist when you blink your eyelids. Tears also protect the eye from bacteria and other germs. They wash away dust and debris to prevent irritation and infections. Closing your eyelids when something is coming towards your eyes can protect them from injuries. Certain muscles are responsible for closing and opening the eyelids. They are also used for facial expressions. These muscles are the:
- Orbital part, which surrounds the eye.
- Palpebral part, which is found under the skin of the eyelids.
General Symptoms
Disorders that affect your eyelids can lead to poor vision. It can also make it difficult for you to do daily activities, such as looking at a computer screen or reading.
Common symptoms of disorders that affect the eyelids include:
- Burning or stinging.
- Eye dryness or itching.
- Eye redness.
- Pain or inflammation.
- Crusts that form on the eyelashes.
- Inability to move the eye or blurred vision.
- Sensitivity to light.
Sometimes, eyelid disorders are a symptom of another condition. For example, eyelid drooping may be the result of:
- Brain tumour or cancer.
- Diabetes.
- Injury.
- Stroke.
Contact your health care provider if you have eyelid problems that do not get better after a week, or if you experience:
- An unusual freckle, bump or growth on your eyelid that may change shape or colour.
- Discharge.
- Eyelid drooping.
- The swelling and complete closing of the eyelid.
Blepharospasm
Blepharospasm is one common eyelid disorder. It causes the eyelid to have blinking spasms. The spasms often happen during the day and not while a person is sleeping. İt is a form of dystonia, a movement disorder. It causes muscle contractions which result in sustained eyelid closure, twitching or repetitive movements. This can affect a person’s ability to see. The symptoms of blepharospasm begin slowly. The frequency of eye blinking often increases over time, especially when the eye is irritated. Eventually, the eyelids may remain closed for long periods. Daily life can be greatly affected. Blepharospasm happens in both men and women. It is most common in middle-aged or elderly women. Treatment for blepharospasm may include:
- Botulinum toxin injections which relax the muscles and stop the spasms.
- Medicines
- Surgery, either of the eye muscles or deep brain stimulation surgery.
Blepharospasm may worsen or expand to surrounding muscles. It may remain the same for many years. Rarely, the condition may improve suddenly on its own.
Blepharitis
Blepharitis is the inflammation of the outer edges of the eyelids near the eyelashes. It happens when too much oil is made by the glands near the eyelids. Other possible causes of blepharitis include:
- Bacterial eye infections.
- Certain types of skin conditions, such as acne rosacea.
- Dry eyes.
Blepharitis can cause the following symptoms:
- A burning sensation.
- Blurred vision.
- Crusting.
- Frothy tears.
- Red and swollen eyelids.
It can be difficult to manage. This is because the condition often comes back after it is treated. Treatment for blepharitis focuses on home care, including:
- A special diet and nutritional supplements.
- Good hygiene.
- Scrubbing around the eyes with a clean washcloth or cotton swab.
- Warm compresses to loosen crusting.
Antibiotic ointment may also be prescribed. This can help get rid of the bacteria causing blepharitis. Steroid eye drops or artificial tears can also be used. These help control inflammation and relieve dry eyes.
Cancer
Problems that affect the eyelid or the eyelid skin may be caused by cancer. Cancer begins in your cells, the building blocks of your body. Normally, your body forms new cells as you need them, replacing old cells that die. Sometimes this process goes wrong and tumour forms. If a tumour is a cancer, cells from the tumour can invade other tissues throughout the body. Cancer cells can spread to different parts of the body through blood vessels and lymph channels. Types of cancer that may affect the eyelid include:
- Basal cell carcinoma.
- Squamous cell carcinoma.
- Sebaceous gland carcinoma.
- Malignant melanoma.
Malignant, or cancerous, eyelid tumours can damage the structure of the eyelid. They can also cause you to lose your eyelashes. Treatment for cancers that affect the eyelids may include:
- Surgery.
- Chemotherapy.
- Radiation therapy.
- Photodynamic therapy.
- Biological therapy.
Other Eyelid Disorders
Many other conditions can affect the eyelids. This section discusses additional common eyelid disorders. Dry eye happens when the eye does not make tears correctly. Untreated, dry eye can cause inflammation, eye pain or scars on the cornea. It may also cause loss of vision. But this is not usually permanent. Dry eye can be a side effect of some medicines. It can also be caused by skin diseases on or around the eyelids and diseases that affect the glands in the eyelids. Artificial tears, gels and ointments are available over-the-counter to treat eyes that are dry or inflamed.
Use an indoor air cleaner to filter dust and other particles to help prevent dry eyes. A humidifier may also help by adding moisture to the air. Bacterial infections can affect the eye. For example, styes are red, tender bumps that happen on the eyelid. They are caused by a bacterial infection of the eyelid’s oil glands. Hordeola are swellings that happen under the eyelid. They are common and are caused by a staphylococcal infection. If an eyelid infection takes longer than 2 weeks to get better, antibiotics usually can treat it.
Anti-inflammatory medicines can treat eyelid swelling. Medicines can also increase tear production and prevent damage to the cornea. As you age, your eyelids stretch. The tissue structures and muscles that support your eyelids weaken. The skin may start to sag. This may cause drooping eyelids. Eyelid surgery, also known as blepharoplasty, is a procedure to repair droopy eyelids. It removes excess skin, muscle and fat. You might consider it if drooping or sagging eyelids:
- Keep your eyes from opening completely.
- Impair your vision.
- Pull your lower eyelids down.